ASHCROFT LEADS
- Doctor: Dr Liz Hamblin
- Nurse: Kay Brigg
- Admin: Chris Rushton & Tracey Firth
DATE REVIEWED:
20th June 2019
DATE OF NEXT REVIEW:
June 2020
The Policy/Protocol
This surgery is committed to lessoning the risk and so control of infection within the building and in relation to the clinical procedures carried out within it. The practice will undertake to maintain the premises, equipment, drugs and procedures to the standards detailed below and will undertake to provide facilities and the financial resources to ensure that all reasonable steps are taken to reduce or remove all infection risk. Wherever possible or practicable the practice will seek to use washable or disposable materials for items such as soft furnishings and consumables, e.g. seating materials, wall coverings including paint, bedding, couch rolls, modesty sheets, bed curtains, floor coverings, towels etc, and ensure that these are laundered, cleaned or changed frequently to minimise risk of infection.
- Please remember that patient and staff safety is EVERYONE’S responsibility. So – report anything you think that is not clean, dangerous or risky to a senior member of staff (Practice Manager/Assistant Practice Manager in the first instance).
- The spillage bucket is under the stairs store – this includes a mercury spill kit, body fluids/blood kit, anti bacterial spray and a steam mop.
- Keep the building tidy. This is also for fire risk reasons – the last thing we want is obstacles in the way. If you see anything obstructing the fire exit, please remove it immediately and let the Practice Manager know.
- Remember to wash your hands – it’s one of the easiest ways to stop infections from spreading. There are detailed guides on how to wash your hands properly in the toilets and in clinical areas. Don’t forget to use the antiseptic handwash gels provided throughout the building.
- The Accident Book is kept in the post room – hanging from a hook on the end of the shelf. This book is to be returned to that position and not removed from that room. If you make an entry into it, please inform the Practice Manager the same or next working day.
The Spillage Kit
- This is located in the cupboard under the stairs. It consists of a black bucket, gloves, goggles, antiseptic granules and a steam mop.
In a Major Accident or Incident
- Occasionally, personnel will be involved with a major incident or accident where many people are injured, possibly seriously.
- All personnel are to take reasonable steps to protect themselves from injury and contamination. However, it is recognised that this may fall far short of the guidelines below.
- Personnel should remember that their prime duty under these circumstances is to the patient whilst maintaining as many safety precautions as possible. For this reason, vaccination with the Hepatitis B vaccine is mandatory for all medical personnel.
Occupational Health
Practice area
Contact details / address
Bradford & Airedale
Needlestick Injuries – telephone 0247 630 9727
Pre-placement questionnaires, case management referrals and vaccination / immunisation bookings:
email info-occhealth@sugarmanhealth.com or telephone 0247 630 9727
Leeds
Needlestick Injuries – telephone 0247 630 9727
Pre-placement questionnaires, case management referrals and vaccination / immunisation bookings:
email info-occhealth@sugarmanhealth.com or telephone 0247 630 9727
Calderdale & Kirklees
Tel: 01484 226424
Email: employee.healthcare@kirklees.gov.uk
Employee Healthcare
Rowan Bank
Claremont Street
HuddersfieldHD1 5BY
Wakefield District
Tel: 01924 316031
Email: occupational.health@swyt.nhs.uk
Occupational Health & Wellbeing
Block 11
Fieldhead Hospital
Ouchthorpe Lane
Wakefield
WF1 3SP
Click here for our Occupational Health page: https://www.ashcroftsurgery.co.uk/occupational-health/
Specific Infection Control Protocols
The following measures to be taken by all staff to limit the risks of infection from the following biological substances. Each individual member of staff has personal responsibility for becoming familiar with these.
 It is essential that everyone working in clinical environment is aware of the risk from contaminated needles. You should be aware of the policy even if you do not use needles in your own work.
It is essential that everyone working in clinical environment is aware of the risk from contaminated needles. You should be aware of the policy even if you do not use needles in your own work.
Important Rules
- Never bend or break needles
- Never re-sheath needles by hand
- Discard all needles into a designated box
- Never disconnect the syringe from a needle
A Quick Reminder of Important Preventative Measures
- Sharps should be kept in the appropriate “Sharps” box, out of the reach of children and with the lid closed. No sharps box should be kept at floor level or at a level where a child can reach into it easily. This is everyone’s responsibility. If you see a sharps bin at a risky place, move it to a secure place and inform the Practice Manager and Nurse Leads.
- Sharps should be disposed of by the person using them. Never leave sharps to be disposed of by someone else.
- Never stick you hand into the sharps bin when disposing of the sharp. Drop it in safely.
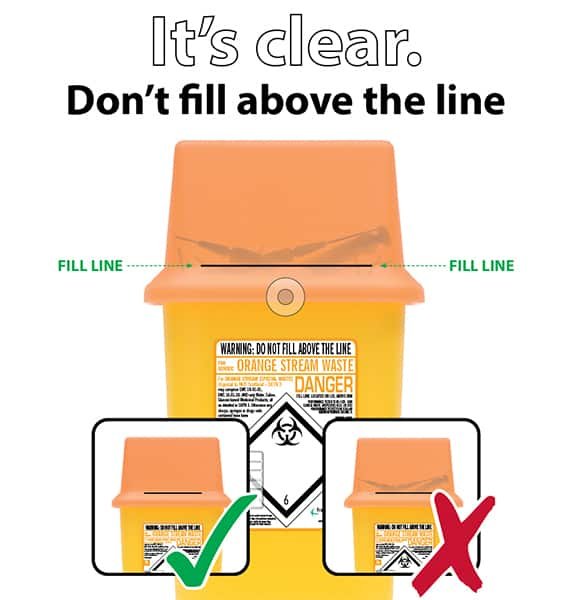
- Sharps bins should not be overfilled. Needles and things should NOT be sticking out of the entrance hole at the top. Boxes must only be filled to the manufacturers’ line and should be disposed of every three months, even if they are not full. Make sure NEEDLES AND SHARPS DO NOT GO ABOVE THE FILL LINE.
If you are subject to a needlestick injury or human bite…
Blood should be taken and tested within 24 hours. Tests are needed whether or not you have been vaccinated against Hepatitis B.
- Immediately
- Make the wound bleed, if possible.
- Clean well with copious amounts of soap and running water.
- Apply occlusive dressing.
- Identify the source of the sharp.
- Contact Clinical Lead within the practice – see above for Nurse, Doctor and Admin leads.
- It is the responsibility of staff suffering injury to ensure that advice on First Aid is sought and to ensure completion of the appropriate documentation in accordance with the Health and Safety Regulations.
Clinical Lead/GP Action….
- Re-emphasise above actions
- Please liaise Airedale Hospital Occupational Health Department: 01535-294401.
- Follow this flowchart in the case of a needlestick injury. (the number on this flow chart is wrong – we now use Airedale Hospital Occupational Health Tel: 01535-294401. )
- In particular
- Identify the patient and the member of staff affected.
- Take a focused history to identify risk of HIV, HEP B (HBV) and HEP C (HCV). Note the type of injury, depth, gauge of needle, if used for injecting or aspiration, and if hollow bore or bloodstained.
- Take blood – in particular: HIV, Hep B, Hep C. Counsel and consent patient and member of staff that blood will be tested for HIV, Hep B and Hep C.
- If high risk for HIV: start Post Exposure Prophylaxis (preferably within an hour, but worthwhile up to 36 hours post-exposure). Send them to A&E at BRI or AGH for Post Exposure Prophylaxis (within 1 hour of incident if possible).
- Find HBV status of “recipient” and consider booster even if good immunity, consider HEP B immunoglobulins. If immunoglobulin is required, the member of staff will be contacted and treated by the Accident and Emergency Unit. Immunoglobulin must be given within 48 hours to be of most benefit.
- Repeat blood tests will be need in 3 months time from both patient and member of staff – counsel them. HIV testing is not routine and will not be undertaken without full counselling.
- An accident report should be completed – find the accident book. Also send email to notify both the Practice Manager and Lead Nurse of the incident with details for follow up. Details in the yellow section above.
What to record in the Accident Book/email to the leads
The Accident Book is kept in the post room – hanging from a hook on the end of the shelf. This book is to be returned to that position and not removed from that room. If you make an entry into it, please inform the Practice Manager the same or next working day.
- The source of the Sharp and description of the accident, including the place, date, time and any witnesses.
- The name of the source patient.
- The action taken.
- Any persons who gave advice and the advice given.
- The advice given to the patient and / or staff member concerned.
- The action taken to prevent recurrence.
Further Information
Advice about blood taking also applies to vaccination of patients. Always avoid contact with blood by the use of cotton wool swabs after withdrawing the needle. Never sheathe the needle, always dispose of needles safely and without delay. When disposing of the needle it is to remain attached to the syringe, unlike blood letting where the purpose of removing the needle is to avoid haemolysis of the blood cells.
- If there is spillage within the workplace a spillage kit is available (LOCATED IN THE UNDER STAIRS CUPBOARD BLACK BUCKET AND STEAM MOP) containing antiseptic granules which may be poured onto blood spills, leave for 2 minutes, and removed using paper towels. The kit also contains gloves (to be replaced if used once) and goggles to prevent splashes into the eyes. Disposable aprons should also be used.
- If there is any blood or other body fluid spillage outside the workplace then it can be rinsed away with a 2% bleach / water solution.
- Block off spillage areas from patients and staff until the spillage has been removed. Always use Personal Protective Equipment (PPE), and note the following general guidelines:
- Paper towels etc, once used, should be placed in clinical waste
- Non-disposable items such as buckets etc should be disinfected using a suitable bleach / disinfectant solution
- All used PPE should be disposed of as clinical waste
- Always wash your hands using thorough techniques immediately after the event – POSTERS OF THE HAND WASHING PROCESS CAN BE FOUND AT EACH HAND WASHING AND GEL POINTS.
Notes:
- HIV is much less infectious than Hep B. HIV will not live long outside the human body but Hep B will survive for over a week in a drop of dried up blood. Consequently everyone in the practice will receive a Hep B vaccination shortly after recruitment, and everyone will receive training on infection control on an annual basis.
- In the case of possible acute infection by a HIV+ patient, drugs are available which, if administered within 1 hour will give an 80%+ chance of killing the HIV infection. In such cases, the A&E department is to be contacted immediately for advice on obtaining this treatment (which is called Post Exposure Prophylaxis – PEP for short).
Two major potential hazards from blood are contraction of Hepatitis B and C and the AIDS virus. The risk of contracting any of these is minimal if the operator does not inject his or her self with the patient’s blood. If the operator has an open wound and spills an infected patient’s blood there is a potential for transmission of one of these infective agents; in these circumstances it is advisable that the operator wears gloves. Medical personnel who either handle blood samples or take blood from patients are therefore to take the following precautions.
The situation of a patient who is bleeding rarely poses a significant risk to the staff. However, some risk does exist and extra precautions and therefore needed:
- Always wear gloves when dealing with open wounds whether or not they have stopped bleeding.
- In the event of significant bleeding, such that would lead to contamination of medical staff clothing, a plastic apron must be worn.
- Patients should not leave the Practice whilst they are still bleeding as this poses a risk to the general public.
- Contaminated clothing belonging to the patient should be placed inside a plastic bag and returned to the patient with appropriate advice about soaking clothing in cold water before washing and about prevention of contamination of the clothing of other personnel. The patient should be advised to disinfect the bowl or sink that the clothing is soaked in.
Two major potential hazards from blood are contraction of Hepatitis B and C and the AIDS virus. The risk of contracting any of these is minimal if the operator does not inject his or her self with the patient’s blood. If the operator has an open wound and spills an infected patient’s blood there is a potential for transmission of one of these infective agents; in these circumstances it is advisable that the operator wears gloves. Medical personnel who either handle blood samples or take blood from patients are therefore to take the following precautions:
Handling of Samples:
- All samples of blood are to be in the approved sample tubes provided, which are sealed by a top. Should leakage of blood occur due to imperfections in the bottle or incorrect fitting of the top, the sample is not to be transported out of the practice in the container.
- All sample tubes containing blood are to be inserted into an approved plastic bag, which should be sealed to minimise the risk of contamination of personnel should leakage occur.
- If there is a leak or spill the action will depend on the extent of the leak. If the leak is contained within the plastic bag the bag should not be opened and should be inserted within another plastic bag, which should then be sealed. A suitable person (doctor/nurse) is to be informed if a leak occurs and will decide whether to dispose of the sample or to transfer the remains of the sample into another bottle. The transfer of blood should only be undertaken when the risk of contamination of personnel is minimal and when gloves are used. Otherwise the sample is to be disposed of as above in a plastic bag inserted to the clinical waste container.
- If the leak is not contained within the bag and contaminates either the outside of the bag or external objects the following action is to be taken:
- Avoid any further contamination by containing the sample within another plastic bag – if possible without undoing the bag. Tighten the top of the tube as this may be loose.
- Dispose of the sample within an approved clinical waste container.
- Ensure that your hands are washed thoroughly with hot water and/or alcohol gel or soap. Any cut or open wound that comes into contact with the patient’s blood should be thoroughly washed to ensure that none of the patient’s blood remains in contact with the wound. Hand washing notices are located at each hand washing sink and gel point.
- Any contaminated objects should be cleaned and disinfected as described below.
- All blood should be treated as high risk and universal precautions applied.
It is important to highlight those samples which require special handling because of their infection risk to others; we have a duty to protect our laboratory staff. Such samples should be labelled (with a ‘Danger of Infection’ label) to alert laboratory staff that the specimen requires special handling. Clinical judgement is required in deciding to label samples correctly, and the onus is on the requestor to label correctly. Samples from the following will require a ‘Danger of Infection’ labelling:
- Patients with proven infection with a Hazard Group 3 (HG3) pathogen. For example…
- Hepatitis B and C
- HIV
- Tuberculosis and other mycobacteria
- Typhoid
- Brucella
- Anthrax.
- Patients suspected of having a HG3 pathogen (information from clinical history and examination e.g. injecting drug user, haemophiliac, vCJD)
- A patient who is part of an ongoing outbreak caused by HG3 pathogen.
Inmates of prisons.
Two major potential hazards from blood are contraction of Hepatitis B and C and the AIDS virus. The risk of contracting any of these is minimal if the operator does not inject his or her self with the patient’s blood. If the operator has an open wound and spills an infected patient’s blood there is a potential for transmission of one of these infective agents; in these circumstances it is advisable that the operator wears gloves. Medical personnel who either handle blood samples or take blood from patients are therefore to take the following precautions:
The taking of Blood:
The risk of contamination to personnel is always less if the patient and the operator are relaxed and still. It is recommended that patients lie down during blood letting where appropriate. It is imperative that the operator takes his/her time and does not rush. Rushing leads to accidents and mistakes! Sterile disposable syringes and needle are to be used only once. Care is to be taken that no blood comes into contact with the operator’s skin by taking the following precautions:
- Always withdraw the needle from the vein whilst covering the site of the needle puncture with a cotton wool ball (not a medi-swab).
- Should a drop of blood escape from the end of the needle following the withdrawal, allow it to drip into the cotton wool ball.
- Do not sheath the needle as this is the most common cause of needlestick injury.
- If a vacutainer system is not used, carefully pull back on the syringe to draw a little air into it.
- Carefully remove the needle from the syringe/vacutainer holder and place it immediately into the sharps box.
- Where syringe and needle are used, insert the required amount of blood into the bottle and do not fill beyond the line, since this increases the risk of spillage during transportation.
- With the introduction of vacutainers, the risk of spillage from filling bottles has diminished but care still needs to be taken when removing the bottle from the inducer when two or more specimens are needed to be collected.
- Replace the cap on the bottle and ensure a good seal.
- If required the bottle may be mixed with the preservative by gently rolling or tipping the bottle. Do not shake.
- When the required number of bottles has been filled, the syringe and any contents need to be disposed of in the sharps box. This will decrease the risk of spillage of blood onto the outside of the container from the syringe.
- If the amount of surplus blood in the syringe is more that 5 mls it should first be sealed in a blood bottle, and then discarded.
- Once the sharps box is two thirds full it is to be sealed and returned for disposal. Under no circumstances attempt to force a syringe into a sharps box.
- All specimens are to be sealed in plastic pathology sample bags ready for transportation. Each sample should have its own bag. All forms that accompany the sample should be in a separate part of the plastic bag.
- Specimens should be stored in a cool safe place.
- All personnel who work with or may handle blood or pathological specimens are to be vaccinated against Hepatitis B and have their antibodies measured following vaccination to reduce the risk of contracting this infection.
 Sharps Boxes:
Sharps Boxes:
The purpose of a sharps box is to protect personnel from injury. The most likely time that injury will occur is when inserting an object into the sharps box. Therefore it is important that the box is not used beyond the two-thirds full stage. If the box is more that two thirds full, seal it and start a new box. And remember – never force objects into the box – if the syringe is too big to fit into the box, even though the box is not yet two thirds full, start a fresh box.
- Always ensure that sharps and sharps boxes are well out of the reach of children who might venture into the treatment room.
- More advice under the Needlestick Injury Protocol below
Urine, whether non-infected or infected, poses less of a risk than blood. However sensible precautions should still be taken to avoid contamination of personnel or their clothing. Gloves should be worn when handling urine containers as it is impossible to tell whether or not the container is contaminated with blood or faeces.
Urine Samples in Sealed Containers
- Samples of urine in sealed containers should pose no health risk provided that the bottle is adequately sealed and no urine contaminates the outside of the bottle.
Analysis of Samples of Urine
- Pregnancy tests and dipstick testing make necessary the opening of urine bottles and exposure of personnel to urine. Gloves should be worn whilst testing urine and hands must always be washed after handling urine and testing urine.
- Disposal of Urine. Urine is to be disposed of down the sluice or toilet. Under no circumstances may it to be disposed of down a sink.
- Disposal of Urine Containers. Urine containers are disposable and are to be used once only. Urine bottles are to be emptied when analysis is complete, rinsed and the bottle resealed and disposed of in the clinical waste bin.
Faeces pose a risk to medical personnel. Through faeces a number of diseases are transmitted that can be serious (though they are rarely as serious as blood diseases). It is important to handle specimens correctly to avoid the risk of disease.
Samples:
- Samples should be handed in inside a blue top specimen pot. Other containers are not acceptable. The patient should label his specimen container before defecation with his name, date of birth and date and time of production. The specimen should then be placed inside a specimen bag and sealed by the patient. The patient should be advised to wash his hands thoroughly after defecation before touching the specimen pot and again after inserting the specimen pot into the bag.
- The cleaners will clean the toilets 5 times a week. In the event of a patient having diarrhoea the toilet should be cleaned by the patient if they are well enough, or by medical staff in the event of the patient being too ill to perform this task. Medical staff and cleaners should wear gloves when cleaning the toilet. Hands must always be washed afterwards.
- Vomit can contain infective organisms and is thus a risk to personnel. Always work on the assumption that the vomit is infected. Patients will usually have time to obtain a bowl or find their way to the toilet, but occasionally patients will vomit on the floor or furnishings.
- Disposable paper bowls are available in reception, but if any other container is used it should be emptied down the sluice or toilet and washed out immediately after being emptied and then disinfected. Toilets should be cleaned and sterilised in the same way that they are for diarrhoea. Personal Protective Equipment should be used. Spillages are to be cleaned in accordance with the practice spillage guidelines within this document.
Sputum should be collected by the patient into a universal container and labelled by the patient. The container should be inserted into a plastic specimen bag with the request form in the pocket separate to the specimen itself. In the event of the specimen leaking out of the bottle or the bottle breaking the specimen is to be disposed of and a new specimen obtained.
Swabs are taken of many infected areas of the body to assess the cause of the infection. Thus a swab by definition contains an unknown hazard. Provided the swab is not removed from the transport medium, no risk of transmission of infection exists unless there has been contamination of the outside of the container. The following guidelines are to be followed:
Taking Swabs from Infected Lesions:
- The infected area must not be touched with the hands.
- The infected area must not come into contact with the operator’s clothes.
- The container for the swab and the patient are to be as close together as is reasonably possible in order to minimise the distance that the swab needs to travel once the specimen has been taken.
- Care is to be taken that the swab contains enough material for analysis but not so much that there is a likelihood of dripping pus during the transit of the swab from the patient to the specimen container.
- The top of the bottle must be sealed adequately before insertion into a sealed plastic hazard bag. The form that accompanies the specimen is to be placed in the appropriate pocket of the bag and not in the same compartment as the specimen.
- In the event of the top becoming loose and parting from the container whilst in the bag, the top is to be re-sealed either through the bag, or by opening the bag.
- The transport medium is solid and unlikely to leak out of the bag, however, in the unlikely event of this occurrence it has to be assumed that microbiological material has also leaked. Therefore the specimen is to be disposed of and re-taken.
Semen should be collected by the patient into a universal container. The patient will usually drop of his sample directly to the place where the analysis occurs. There is usually a time limit between collection and the time it must be delivered to the labs. It must be placed in a plastic bag, accompanied by a completed test request form. Staff at the surgery will not usually be involved in the handling of these samples.
- The doctors and qualified nurses are the only persons permitted to perform vaginal examinations and smears.
- Two types of speculum are currently in use; the disposable speculum and the stainless steel speculum. Disposable specula are to be put in the clinical waste bag after use and this can be done by appropriately trained staff who may be assisting with the procedure. Gloves are to be worn when disposing of these instruments. Used spatula are to be placed in the clinical waste bag. Stainless steel specula are still single use, can be placed in the clinical waste bad if wrapped, placed in its previous practice wrapping. These days, most practices do not use stainless steel specula.
- Cervical smear specimens are to be placed upon a collection box to dry following collection or directly into the slide specimen box.
General Measures
Precautions should always be taken to avoid contamination of clothing whenever possible, by the use of protective clothing, e.g. plastic apron when the situation can be anticipated. However there will be occasions when it is difficult to anticipate the situation. Contamination of clothes with biological material necessitates the following measures:
- Remove as much surplus material as possible using gloves and a disposable wipe.
- Change into clean clothing if there exists any risk to either the operator or patients whom the operator will treat during that shift. If in doubt – change.
- Personnel should ensure that the clothing does not come into contact with any surface on which food is prepared.
- Blood stained clothing should be soaked in cold water prior to washing to facilitate removal of the stain.
- Soiled clothing should ideally be washed separately from other non-soiled clothing and the washer used at the maximum temperature that the clothing could tolerate without being damaged.
- There may be occasions when it is deemed fit for an item of clothing to be destroyed due to contamination with biological material. Under these circumstances the item is to be sealed in a hazard bag and disposed of in the clinical waste bin.
- Biological or clinical waste is to be placed in appropriate containers only. Sharps are to be placed only in sharps boxes. Only contaminated material that cannot penetrate the plastic is to be placed in hazard bags. Contaminated or non-contaminated material that may penetrate the hazard bags most be placed in a sharps box. This includes unbroken glass that may become broken if the bag is damaged in transit.
- Yellow hazard bags are to have no contamination of their outer surface. If there is contamination of the outer surface of the bag with biological material, the bag is to be placed inside another bag and sealed ready for transportation.
- Once boxed or bagged in hazard containers, waste is to be stored in the Clinical Waste bin. The waste material is to remain inside these solid containers until collected by the clinical waste contractor.
- The surgery has a contact with a cleaning organisation to perform a general clean daily.
- The couch curtains will be cleaned every 6 months.
- The practice will recieve a deep clean every 6 months.
- Hand washing posters will be displayed at each designated hand basin and gel point.
- Infection Control training will take place for all staff on an annual basis and will include hand washing procedures.
- Infection Control information will be included in new staff induction and thereafter in the practice’s annual training process.
- Random and unannounced infection control inspections by the above named staff will take place on a bi-yearly basis and any areas of concern reported to the doctors meeting for (any) remedial action.
